Diaper rash is any rash affecting the skin covered by a diaper. Other names for diaper rash are “diaper dermatitis” or “napkin dermatitis”.
WHAT CAUSES DIAPER RASH?
Diaper rash is usually caused by wetness and friction. Urine and stool (pee and poop) can cause even more irritation, and this leads to breakdown of the skin. Products used to clean the skin can sometimes add to the irritation.
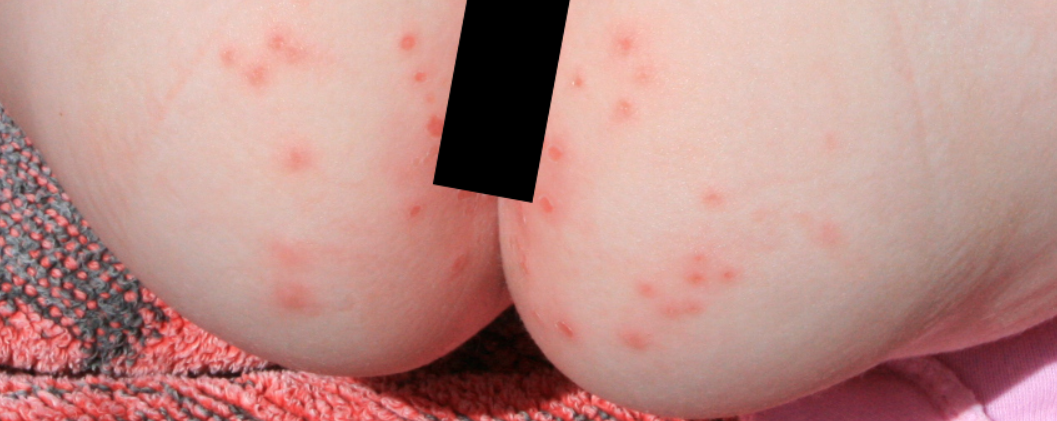
Once the skin under the diaper becomes irritated, germs like bacteria and yeast can infect the skin and worsen the rash.
In some cases, other skin conditions, like psoriasis, can be worsened or triggered by diaper rash.
Signs:
Any rash in the diaper area, ranging from mild to severe.
The skin may be:
- red
- scaly
- painful
- covered in red bumps
- covered in open sores
WHO GETS DIAPER RASH?
Diaper rash is most common in newborns and infants, but anyone who needs to wear a diaper can develop this rash. About one-half of all babies develop diaper rash at some time during the first year or two of life. Diaper rash is most common between 9 and 12 months of age.
Diaper rash is more common when the child is having frequent bowel movements or diarrhea. An illness, a medication like an antibiotic, or a change in diet can cause changes in bowel movements.
PREVENTING DIAPER RASH
- Change diapers frequently.
- Use superabsorbent disposable diapers to keep the skin under the diaper as dry as possible.
- Wipes:
- Cleanse the skin gently rather than scrubbing. Do not overdo it! Too much cleaning can actually irritate the skin, particularly when harsh soaps or chemicals from wipes are involved.
- Soft cloths moistened with plain water are the gentlest because they do not contain chemicals.
- If you choose packaged wipes, choose wipes that are alcohol-free, fragrance-free, and free of essential oils.
- Barrier diaper creams, pastes and ointments:
- A diaper cream, paste or ointment is called a barrier cream because it protects the skin from urine and stool. If you apply a diaper cream to your hand and wash your hand, you will notice the water beads up and does not get to your skin. In the same way, the diaper cream will protect your baby’s skin from urine and stool.
- Choose only products that are fragrance-free.
- Apply thick amounts of a diaper cream to the skin to protect the area after every diaper change. You do not need to clean off cream left on the skin if the child has not stooled.
- A cream or paste containing zinc oxide (thick and white) is often the best barrier.
- A plain white petroleum jelly or ointment is another good barrier.
- To wipe off the sticky diaper cream when the child is soiled, it helps to use mineral oil on a cotton ball.
- A daily short bath in lukewarm water helps to prevent skin breakdown. Use only gentle cleansers that are fragrance-free. Avoid bubble bath.
TREATING DIAPER RASH
When your child has a diaper rash, you need to follow the directions under PREVENTING DIAPER RASH and take the steps described here. It is very important to stick with the treatment plan for at least a week or two, because diaper rashes take time to heal.
Diapers:
- It is important to use superabsorbent disposable diapers and not cloth diapers when there is a diaper rash.
- Sometimes babies are allergic to the dyes in diapers. If your baby gets a lot of rashes, try switching to a plain white, dye-free, disposable diaper.
Medicated creams:
- Common prescription creams for diaper rashes treat yeast like candida, bacteria like staph or strep, and redness.
- If your doctor prescribes a medicated cream to treat the diaper rash, apply it directly to the skin after cleaning the skin gently.
- Only use the medicated cream as often as your doctor tells you to. These usually need to be reapplied 2 or 3 times a day. If you are given a steroid cream (such as hydrocortisone) you should not use it more than the doctor recommends; this cream is usually used for only a week or two.
Barrier diaper creams:
- Apply a barrier cream (with zinc oxide or petroleum jelly) over the medicated cream. Use the barrier cream as many times a day as possible. You cannot use too much barrier cream. Put the cream on thick so that the urine or stool can never touch the baby’s skin.
- When you change the diaper, if the diaper cream is still there and not soiled by stool, you don’t have to wipe it all away. Simply apply more cream on top. When the cream is soiled by stool, it can be gently wiped away with mineral oil on a cotton ball followed by gently cleaning the skin with a soft cloth and warm water.
- The barrier diaper cream should be applied to the skin in a thick layer after every diaper change.
Wipes:
- It is best not to use packaged diaper wipes while your baby has a rash. Instead, use a soft white cloth with warm water to gently clean the skin. When changing diapers that only contain urine, simply pat the skin dry and reapply the barrier diaper cream.
- It is very important not to scrub the diaper area.

WHEN TO SEE THE DOCTOR
- Rarely, diaper rash can be associated with more serious conditions. Go see your primary care provider or a pediatric dermatologist if:
- The diaper rash is not improving after several days
- of careful attention to the instructions above.
- Blisters, pus bumps or open sores develop.
- There are bruises or evidence of bleeding in the area.
- The child is in significant discomfort.
- The rash is spreading to other parts of the body.
- Your child is losing weight, feverish or seems sick.
Contributing SPD Members:
Brea Prindaville, MD, Sarah Stein, MD
Committee Reviewers:
Andrew Krakowski, MD, Sheilagh Maguiness, MD, Erin Mathes, MD
Expert Reviewer:
Sheila Friedlander, MD
Credit to SPD: The Society for Pediatric Dermatology and Wiley Publishing cannot be held responsible for any errors or for any consequences arising from the use of the information contained in this handout. Handout originally published in Pediatric Dermatology: Vol. 35, No. 5 (2018).

1 thought on “5 Essential Facts About Diaper Rash”